By JOHN HOWELL Elaine Lepold, legs up, reclined in the chair beside her bed. Her right knee was bandaged following the surgery she had undergone, and an oxygen tube ran beneath her nose. She was watching Live PD" on television and spooning chocolate"
This item is available in full to subscribers.
We have recently launched a new and improved website. To continue reading, you will need to either log into your subscriber account, or purchase a new subscription.
If you are a current print subscriber, you can set up a free website account by clicking here.
Otherwise, click here to view your options for subscribing.
Please log in to continue |
|
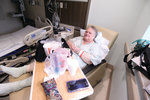


Elaine Lepold, legs up, reclined in the chair beside her bed. Her right knee was bandaged following the surgery she had undergone, and an oxygen tube ran beneath her nose.
She was watching “Live PD” on television and spooning chocolate pudding from a container when she stopped and looked up.
She hadn’t expected visitors.
“People say I must be from Boston because of my accent, but I’m from Lynn,” she said.
Elaine was in unit 2-North at Kent Hospital, ground zero for the relationship-based care implemented by hospital president Robert Haffey soon after his arrival last fall. Elaine, who said she has been a patient in many hospitals, was loving it.
“I asked if I could have coffee and they said, ‘Just call,’” she said incredulously. She made the call and the coffee arrived soon after.
“It’s like room service,” she said.
Elaine’s appraisal couldn’t have been better scripted from the perspective of Nicole Hebert, nursing director of 2-North and 4-West with a combined total of 37 rooms. But Elaine hadn’t been told a reporter would be visiting, or even that she was in a unit serving as the incubator for hospital-wide implementation of relationship-based care by May 2020.
Hebert is working in tandem with Karen Wholey, who is also a registered nurse and is the professional practice coordinator and interim director of education. She serves in the role of training staff in the delivery of relationship-based care. Her goal is to get hospital staff to view their own actions and reactions from the perspective of the patient.
“How would you feel if you were out on that stretcher?” she asks.
With 10 private rooms, 2-North is the “perfect place” to start the program, Herbert said. The unit is dedicated to orthopedic patients who, for the most part, have undergone hip and knee replacements and spend one or two days in hospital recovery. In terms of care, avoiding falls is on the top of Herbert’s list of concerns. She points out patients in recovery are frequently unaware of how unstable they are and take risks they shouldn’t. Beds and chairs have alarms so the unit staff knows immediately when a patient is up.
But there’s more to it than averting a possible accident. Hebert keeps count of how many days the unit has gone without a fall. The number is posted on a bulletin board, along with the number of fall-less days to beat and other information on the unit’s progress that helps in team building – a core component of relationship-based care.
From the moment a patient is admitted, they learn from a board posted in their room the names of “the team” that will be delivering their care, from environmental services (housekeeping) to the nurses and doctors. Patients are encouraged to call the team member they need. The board also displays the patient’s first name or the nickname they prefer, putting people on a first-name basis.
“We have targeted everyone [all hospital staff] to be a part of it. We are all working on a common goal for the patient,” Wholey said.
When a patient is discharged from the unit, they are sent a “thank you” card wishing them continued good health and signed by members of their team. That simple gesture alone has yielded returns.
One patient, who lives alone, called to report it was the only card he had received all year. There were other calls, emails and notes of appreciation, along with boxes of candy, according to staff members.
The personal connections, Hebert feels, are what is lacking in some hospital settings, where care is reduced to charts, timing and procedures. She reasons that relationship-based care brings nurses back to the reason why they entered the profession.
Housekeeper Liz Ramaglia – the one to be summoned when there is a spill, or to change bed sheets and clean up – is encouraged as well as humbled by the response of patients.
“We don’t ask to be heroes,” she said. “We’re here for them [the patients].”
The principles of relationship-based care – introducing oneself to the patient; using the patient’s preferred name; taking five minutes in each shift to review with the patient their care; touching the patient and always saying “thank you”; and using the mission and vales of the hospital in the delivery of care – appear to be common sense. Hebert sums it up as “treating people with respect.”
That sounds simple enough, yet a number of factors are in play in creating a culture of respect. Patients help measure how the hospital is performing in their response to surveys following their discharge.
The Press Ganey survey used by hospitals across the country asks patients to quantify a variety of factors, from communication with the staff to professionalism and hospital cleanliness. Kent consistently ranks in the 75 percentile and on a couple of occasions has topped 90 percent.
Hebert keeps a close eye on 2-North survey results, posting them and pushing the team to hit the 90s. She observes that steps as simple as calling a patient by their first name and engaging with them briefly can alter their hospital experience.
For Wholey, relationship-based care is all about connecting nurses and their patients.
“We want patients to make Kent the hospital they choose for all their health care,” she said.
Comments
No comments on this item Please log in to comment by clicking here